How to Choose the Best Surgical Wound Dressing for Healing?
Selecting the right Surgical Wound Dressing can significantly impact patient recovery. Dr. Emily Hart, a leading expert in wound management, states, "An appropriate dressing is vital for optimal healing." This highlights the crucial role that surgical dressings play in the healing process.
When choosing a Surgical Wound Dressing, various factors must be considered. The type of wound, its location, and the patient's overall health all influence the choice. A dressing that promotes moisture can aid in faster healing. Conversely, one that is too absorbent may lead to complications. It's important to evaluate each option carefully, even though decisions can feel overwhelming.
Many healthcare professionals report challenges in making the best choices. Sometimes, the available options are not perfect. Dr. Hart emphasizes continuous education, highlighting the need for ongoing research and adaptation in wound care practices. This acknowledgment of imperfection invites clinicians to seek innovative solutions for better patient outcomes.
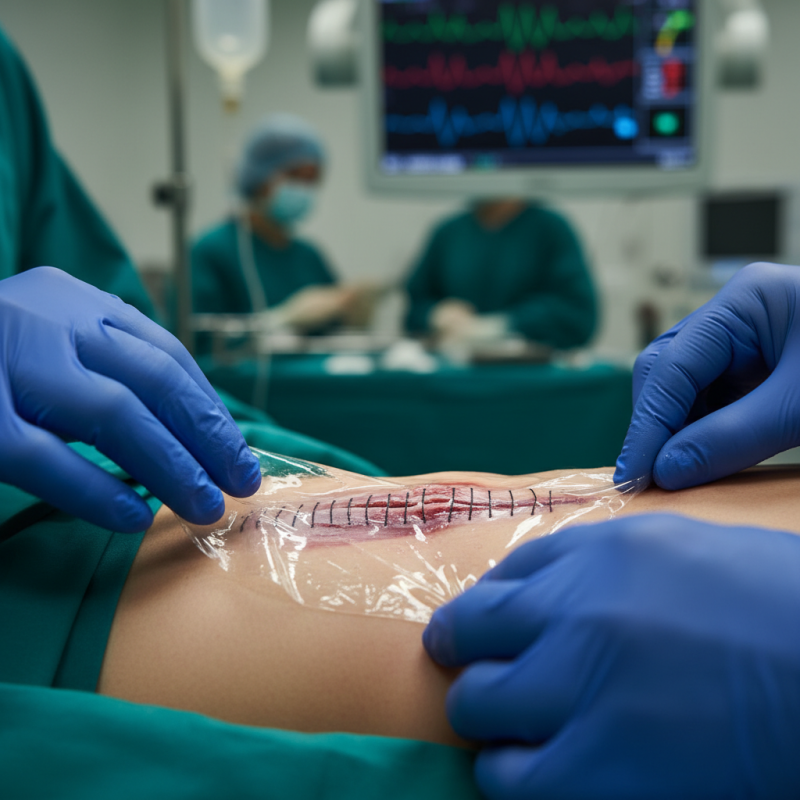
Understanding the Role of Wound Dressings in Surgical Healing
Choosing the right wound dressing is vital for surgical healing. The dressing protects the wound, reduces infection risk, and supports the healing process. Understanding how these dressings function helps in selecting the best option. Wound dressings can be categorized into several types, including transparent films, hydrocolloids, and foam dressings. Each type serves a specific purpose, whether it is moisture retention or protection against contaminants.
Tips for choosing the right dressing include assessing the wound size and depth. Dressings should cover the entire wound area without leaving gaps. Consider the exudate level; some dressings manage moisture better than others. Regularly check the dressing for signs of infection, such as increased redness or pus. Make adjustments if necessary, as not all dressings work for every individual.
Healing takes time, and the choice of dressing can significantly influence this process. Sometimes, a dressing might not perform as expected. Reflect on how the wound responds and adapt your approach. Remember that the goal is to foster an environment that enhances healing while minimizing discomfort. Each wound is unique, and finding the right solution is essential for optimal recovery.
How to Choose the Best Surgical Wound Dressing for Healing?
| Dressing Type | Indications | Benefits | Drawbacks |
|---|---|---|---|
| Hydrocolloid Dressings | Superficial wounds, partial-thickness burns | Moist environment, promotes autolytic debridement | Not suitable for infected wounds |
| Foam Dressings | Moderately to heavily exudating wounds | Absorbent, cushions the wound site | May adhere to wound if moisture is low |
| Hydrogels | Dry wounds, necrotic tissue | Provides moisture, promotes granulation | Requires secondary dressing for better retention |
| Alginate Dressings | Heavily exudating wounds | High absorbency, forms a gel when in contact with exudate | May require frequent changes |
| Transparent Film Dressings | Superficial wounds, IV sites | Allows visualization of the wound, waterproof | Not absorbent, can cause maceration |
Types of Surgical Wound Dressings: An Overview of Options

Choosing the right surgical wound dressing is crucial for patient recovery. There are various types available, each tailored for specific needs. Hydrocolloid dressings, for example, create a moist healing environment. They are ideal for minor to moderate wounds, promoting faster healing. A study by the Journal of Wound Care found that these dressings can shorten healing time by up to 30%.
Advanced dressings like foam absorbers are effective for high-exudate wounds. They provide cushioning and help manage moisture effectively. According to research from the Wound Healing Society, foam dressings can minimize pain during dressing changes, enhancing patient comfort. However, they may not always stick well to very dry skin.
Tips: Choose dressings based on wound type. For example, consider a transparent film for superficial wounds. Monitor the wound condition regularly, as excessive moisture can lead to maceration. Keep in mind that not every dressing will work for every patient, as individual responses can vary significantly. As you assess options, reflect on the specific needs of the wound and the patient's lifestyle for optimal healing outcomes.
Factors to Consider When Choosing a Wound Dressing
When choosing a surgical wound dressing, several factors play a critical role in promoting effective healing. The nature of the wound is paramount. Is it a clean surgical incision or a contaminated one? Each type requires different levels of moisture control and protection to avoid infection. Understanding the specific needs of the wound can prevent complications and aid recovery.
Another important aspect is the level of absorbency. A dressing should manage exudate effectively, which can impact healing. Highly exuding wounds may require more absorbent materials. On the other hand, too much absorption can lead to dryness, hindering the healing process. Finding that balance is crucial and sometimes challenging.
Comfort is equally essential. Patients often struggle with dressings that irritate their skin or restrict movement. A dressing should protect the wound while allowing some degree of flexibility. Not all materials work for every individual. Observing the patient's response is vital. It may take time to find the right dressing that provides both protection and comfort during the healing journey.
Comparison of Wound Dressing Options for Healing
Proper Application Techniques for Surgical Dressings
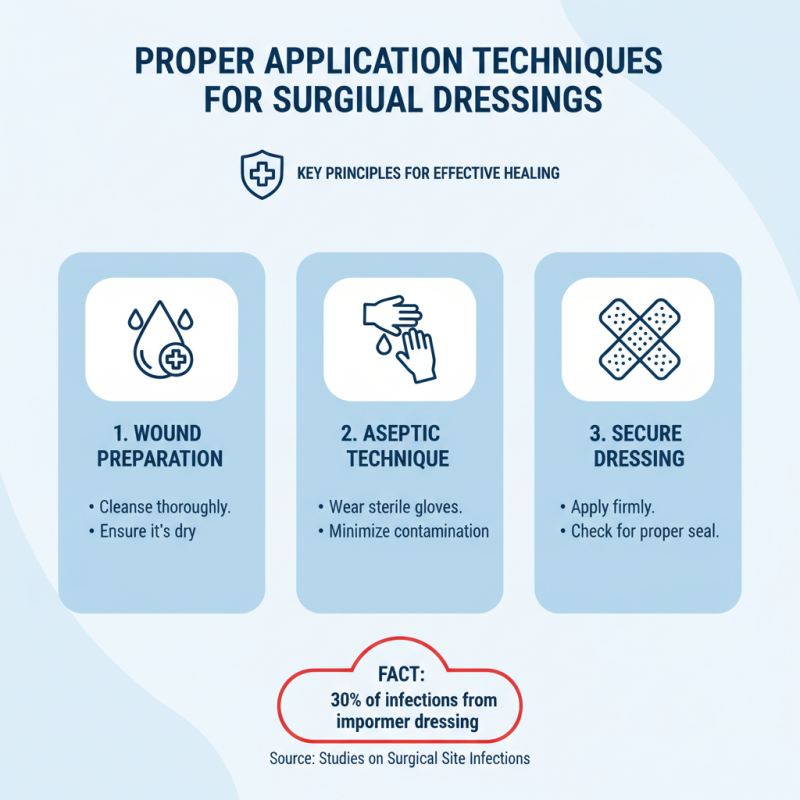
When it comes to surgical wound dressing, proper application techniques are crucial for effective healing. Studies indicate that approximately 30% of surgical site infections can be attributed to improper dressing techniques. Ensure the wound is clean and dry before applying any dressing. Use sterile gloves to minimize contamination risks.
Tips: Always inspect the dressing for any signs of moisture or damage. Change the dressing regularly, typically every 24 to 48 hours, depending on the wound's severity. This helps to maintain a conducive healing environment.
The dressing should fit snugly but not overly tight. Overly tight dressings can impede circulation. Clinical guidelines suggest that the dressing should allow some airflow while protecting against contaminants. Monitoring for any signs of infection, such as increased redness or drainage, is essential.
Tips: Document any changes in the wound's appearance. This can help in evaluating healing progress and adjusting care as needed. Remember, healing can be gradual, and patience is key.
Monitoring and Adjusting Dressings for Optimal Healing
Proper monitoring of surgical wound dressings is crucial for optimal healing. Regular checks allow healthcare providers to assess the wound's condition. This helps identify signs of infection or complications early. Look for redness, swelling, or an unusual odor. Any changes may require adjustments in the dressing type.
Adjusting dressings based on the wound's progress is essential. If the dressing becomes saturated or starts to peel away, it's time to change it. Additionally, evaluate the healing stages regularly. A wound healing slowly may need a more advanced dressing. Conversely, a well-healed wound might need less coverage. Be mindful of how the dressing interacts with the skin. A reactive skin can complicate recovery.
It’s important to document any observations. Keep a record of how the wound progresses over time. This information can inform future dressing choices. Wound healing is not always linear; setbacks may occur. Learning from these experiences can lead to better outcomes. Adjustments based on observation can greatly enhance healing efficiency.
Related Posts
-
Top 10 Surgical Wound Dressing Solutions for Faster Healing and Comfort
-

Unlocking Global Opportunities in Wound Care Management at the 137th Canton Fair 2025
-

2025 Innovations in Wound Care Management: Unveiling Effective Strategies for Global Buyers
-
The Science Behind Wound Dressing: How Proper Techniques Reduce Infection Rates by 50%
-

The Future of Innovative Solutions in Surgical Wound Care
-
Understanding the Importance of Surgical Wound Dressing in Modern Healthcare
